Most Dangerous Microbes On The Planet
The world around us is full of tiny life forms we can’t see with our eyes. Most microbes are harmless or even helpful to humans. But some of these microscopic creatures pack enough power to bring down entire populations. From bacteria that resist all known medicines to viruses that spread like wildfire, these dangerous microbes have shaped human history and continue to threaten us today.
Let’s take a closer look at the most dangerous microbes currently roaming our planet and why they keep scientists awake at night.
Mycobacterium tuberculosis

This bacteria causes tuberculosis, which remains one of the deadliest infectious diseases worldwide. The world’s leading infectious disease with more than 1,700,000 deaths per year, TB affects the lungs mainly but can spread to other parts of the body.
What makes this microbe particularly dangerous is its ability to hide inside human cells for years without causing symptoms. The bacteria then activates when the immune system weakens, making it extremely difficult to eliminate completely.
Drug-resistant strains have made treatment even more challenging, turning what was once a manageable condition into a global health crisis.
MRSA (Methicillin-resistant Staphylococcus aureus)

MRSA, short for Methicillin-resistant Staphylococcus aureus, is a real troublemaker in hospitals. It’s known as a superbug because it’s so hard to kill.
About 1 in 3 people have S. aureus living harmlessly on their skin, but when it becomes resistant to antibiotics, problems start. This ‘superbug’ is very easily spread through human contact and can cause a range of illnesses from skin disorders to deadly diseases like meningitis and pneumonia.
Healthcare workers worry about MRSA because it spreads quickly in hospitals where people are already weak. Simple skin infections can turn deadly when this bacteria gets into the bloodstream or affects vital organs.
Like Go2Tutors’s content? Follow us on MSN.
H5N1 avian influenza virus

Bird flu might sound like something that only affects birds, but H5N1 has proven it can jump to humans with devastating results. Avian influenza A (H5N1), or bird flu, has killed millions of wild birds, and caused sporadic outbreaks among poultry and an ongoing multistate outbreak among cows in the United States.
When humans do get infected, the death rate is extremely high. While the virus generally does not have a severe impact on wild birds, it can be deadly to other animals, including people.
Scientists fear that if this virus learns to spread easily between humans, it could cause a pandemic much worse than COVID-19. The virus keeps changing and adapting, making it a constant threat that requires careful monitoring.
Clostridium difficile
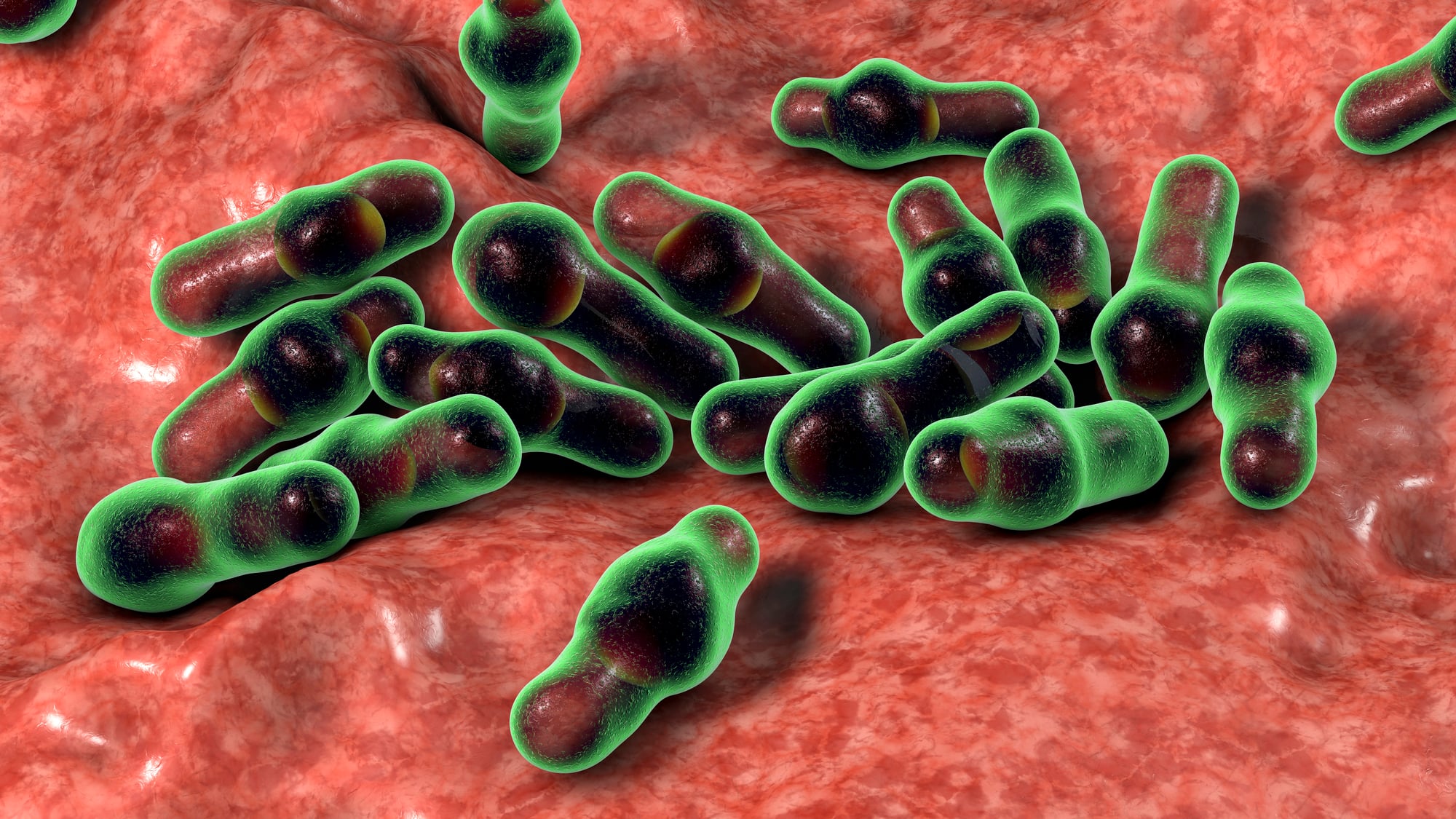
Known simply as C. diff, this bacteria causes severe intestinal infections that can be life-threatening. It normally lives quietly in some people’s guts without causing problems.
But when antibiotics kill off the good bacteria, C. diff takes over and produces toxins that damage the colon. The infection spreads through spores that survive on surfaces for months, making hospitals and nursing homes particularly vulnerable.
What makes C. diff especially dangerous is that it often strikes people who are already sick and taking antibiotics for other conditions. The bacteria has developed resistance to many treatments, and infections keep coming back even after apparent recovery.
Ebola virus

Few viruses inspire as much fear as Ebola, and for good reason. This virus causes severe blood flow both inside and outside the body, leading to organ failure and death in many cases.
Ebola spreads through direct contact with bodily fluids from infected people, making it highly dangerous for healthcare workers and family members. The virus can hide in certain body fluids for months after recovery, creating ongoing transmission risks.
While Ebola outbreaks tend to be localized, they can devastate entire communities before being contained. The high death rate and dramatic symptoms make Ebola one of the most feared microbes on Earth.
Like Go2Tutors’s content? Follow us on MSN.
Carbapenem-resistant Enterobacteriaceae

These bacteria represent a nightmare scenario for modern medicine. CRE bacteria resist carbapenems, which are often called antibiotics of last resort.
When these bacteria cause infections, doctors have very few treatment options left. CRE spreads easily in healthcare settings and can cause infections in the blood, lungs, and other parts of the body.
The bacteria can share their resistance genes with other bacteria, potentially creating even more dangerous strains. Healthy people rarely get CRE infections, but for patients in intensive care units or those with compromised immune systems, these bacteria can be deadly.
The Centers for Disease Control calls CRE an urgent threat to public health.
SARS coronavirus
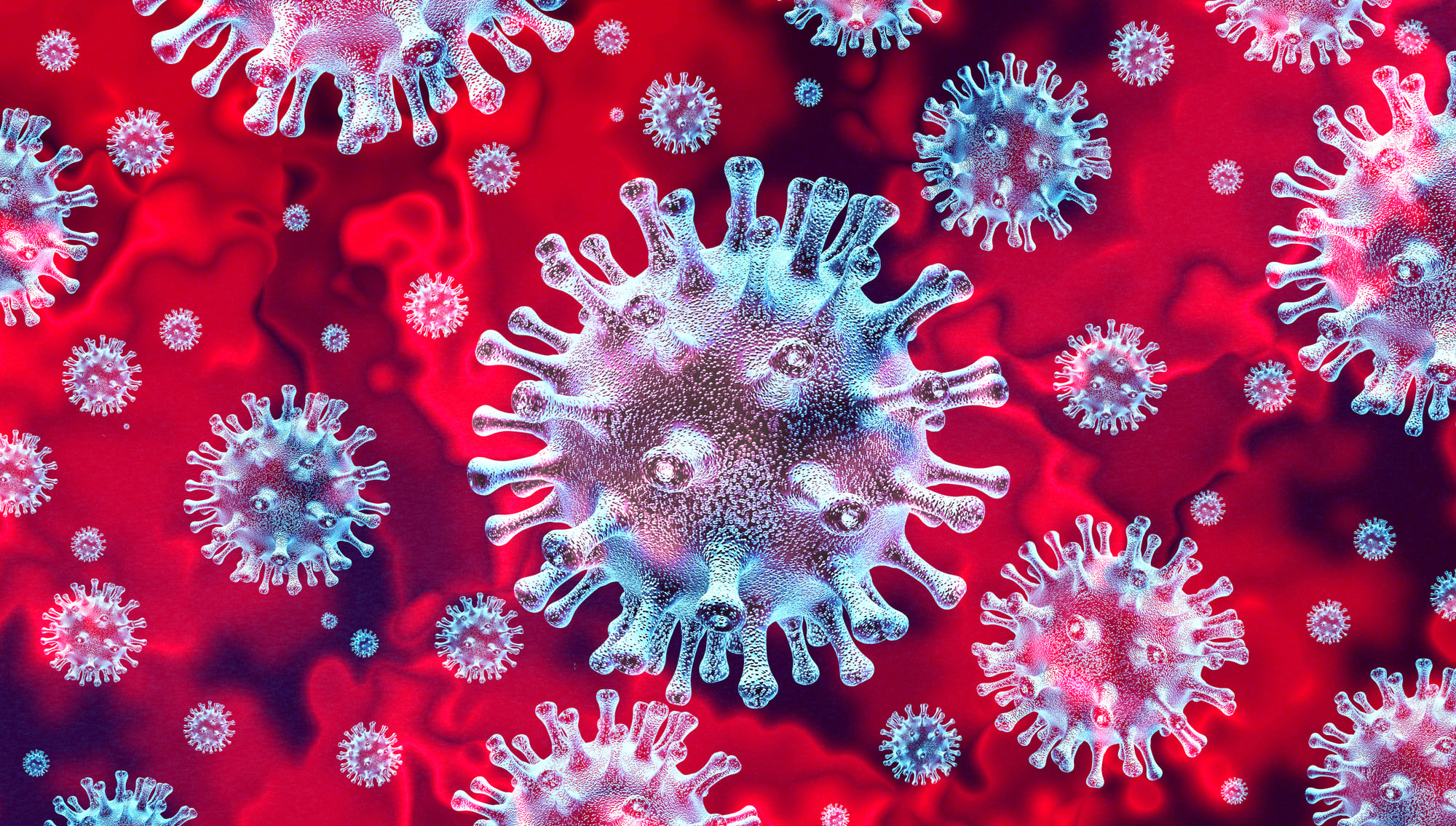
The virus that caused Severe Acute Respiratory Syndrome showed the world how quickly a new microbe can spread globally. SARS appeared suddenly and spread rapidly through international travel, causing severe breathing problems and death in many patients.
What made SARS particularly frightening was its ability to spread in hospitals, infecting healthcare workers who were trying to help patients. The virus seemed to spread more easily than initially thought, creating panic in affected areas.
While SARS was eventually contained, it served as a warning about how dangerous new coronaviruses could be. The experience with SARS helped scientists prepare for future coronavirus outbreaks, though it couldn’t prevent the COVID-19 pandemic.
Neisseria gonorrhoeae

This bacteria causes gonorrhea, a common infection that’s becoming increasingly dangerous due to antibiotic resistance. Drug-resistant strains of Neisseria gonorrhoeae, which causes gonorrhea, are listed as high priority threats by health organizations worldwide.
What starts as a relatively minor infection can lead to serious complications if left untreated or if treatment fails. The bacteria can cause pelvic inflammatory disease, infertility, and increase the risk of HIV infection.
Drug-resistant strains are spreading rapidly, leaving doctors with fewer and fewer treatment options. Some strains now resist almost all available antibiotics, raising fears of untreatable gonorrhea becoming common.
Like Go2Tutors’s content? Follow us on MSN.
Candida auris

This fungus represents a new type of threat in healthcare settings. C. auris was first discovered in 2009 and has since spread to countries around the world.
The fungus resists multiple antifungal drugs, making infections very difficult to treat. It spreads easily in hospitals and can survive on surfaces for weeks.
C. auris often infects people who are already very sick, particularly those in intensive care units. The fungus can enter the bloodstream and spread throughout the body, causing serious infections with high death rates.
Healthcare facilities struggle to control outbreaks because the fungus is so persistent and resistant to cleaning.
Acinetobacter baumannii
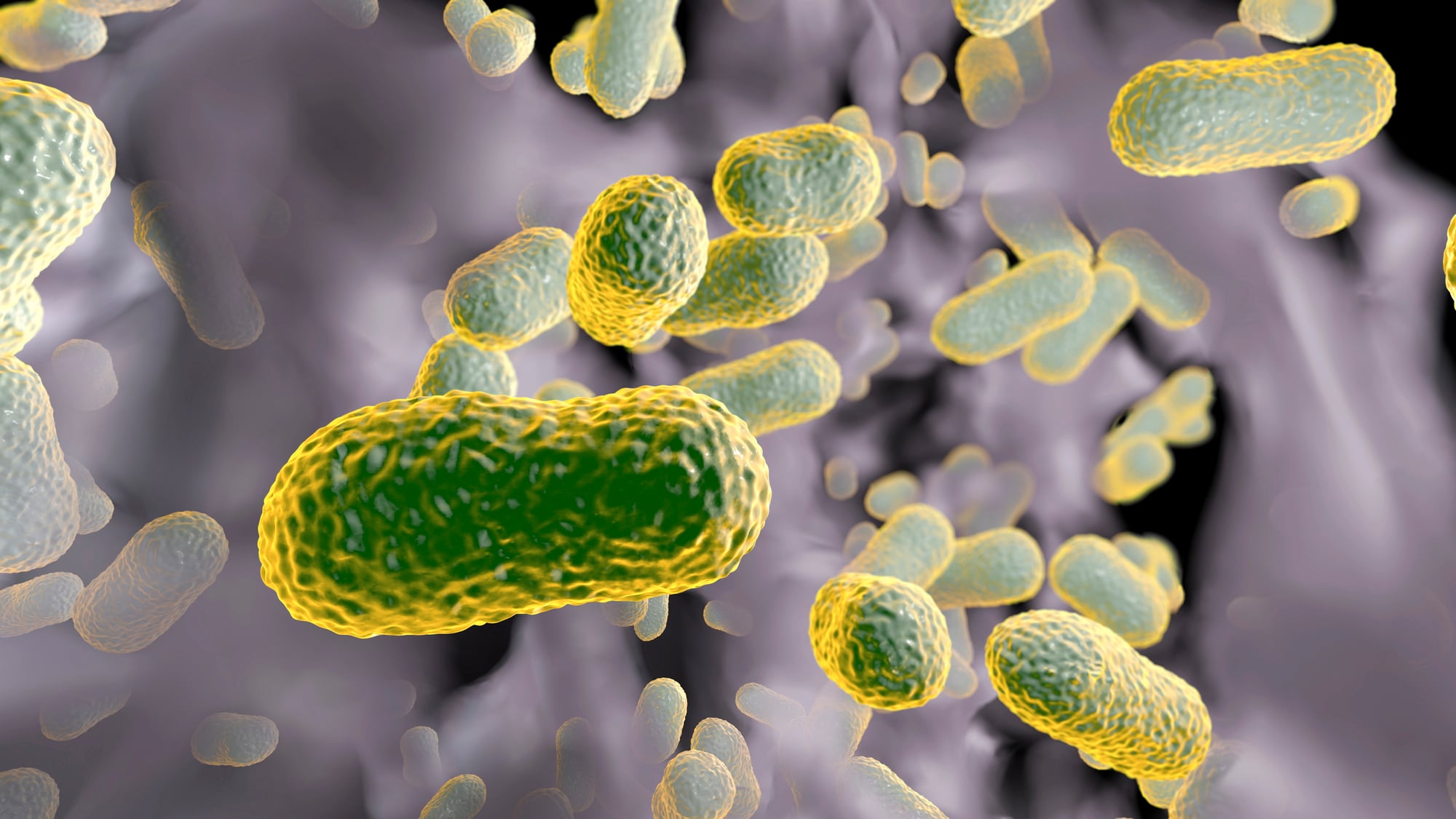
Military hospitals first noticed this bacteria causing serious infections in wounded soldiers. A. baumannii has since become a major problem in civilian hospitals worldwide.
The bacteria resists multiple antibiotics and survives on surfaces for long periods. It particularly affects patients on breathing machines or those with open wounds.
A. baumannii infections are difficult to treat and often come back even after treatment appears successful. The bacteria can cause pneumonia, bloodstream infections, and wound infections that refuse to heal.
Its ability to develop resistance quickly makes it one of the most challenging bacteria facing modern medicine.
Campylobacter jejuni

This bacteria causes more food poisoning cases than any other microbe in many countries. Most people recover from Campylobacter infections within a week, but some develop serious complications.
The bacteria can trigger an autoimmune condition called Guillain-Barre syndrome, which causes temporary paralysis. Food-borne agents like Salmonella and Campylobacter are considered high-priority pathogens.
Campylobacter infections are becoming harder to treat as the bacteria develops resistance to antibiotics. The microbe spreads through contaminated poultry, unpasteurized milk, and contaminated water.
Even though most cases seem mild, the potential for serious complications makes this bacteria a significant public health concern.
Like Go2Tutors’s content? Follow us on MSN.
When past meets present

These harmful microorganisms serve as a reminder that humankind’s relationship with the microscopic world is still complicated and dynamic. Many of these dangers predated modern medicine by a long way, leading to epidemics that influenced the path of history.
Once-susceptible organisms gave way to bacteria that are now resistant to antibiotics. The viruses that decimated populations centuries ago are still resurfacing in new forms that are tailored to our contemporary, interconnected world.
More from Go2Tutors!

- 16 Historical Figures Who Were Nothing Like You Think
- 12 Things Sold in the 80s That Are Now Illegal
- 15 VHS Tapes That Could Be Worth Thousands
- 17 Historical “What Ifs” That Would Have Changed Everything
- 18 TV Shows That Vanished Without a Finale
Like Go2Tutors’s content? Follow us on MSN.



